Retinitis is an inflammatory disease of the retina that can lead to serious vision problems and even blindness. The retina, a thin layered structure lining the back of the eye, is responsible for sensing light and transmitting visual information to the brain. Damage to the retina due to inflammation seriously affects the ability to see.
Inflammation in the retina can occur for a variety of reasons, including infections, autoimmune disorders, and genetic factors. Infections, such as bacteria or viruses, can directly affect the retina, causing it to become inflamed. Autoimmune processes, where the immune system attacks its own tissues, can also cause retinitis. In some cases, the disease has a genetic nature, which causes the development of retinitis in certain families.
The retina is an important component of the visual system, which acts as a kind of "screen" on which the image is projected. It consists of photoreceptors (rods and cones), which convert light signals into nerve impulses. These impulses are then transmitted by the optic nerve to the brain, where they are processed and form a visual image. In retinitis, inflammation can damage these photoreceptors and other cells in the retina, leading to vision impairment or loss.
Retinitis can have a significant impact on patients' quality of life. Symptoms such as reduced visual acuity, the appearance of dark spots in the field of vision, reduced ability to see in low light conditions can limit daily activities. People with retinitis often have difficulty performing simple tasks such as reading, driving a car, or even spatial orientation.
Causes of occurrence
Retinitis is an inflammatory disease of the retina that can have various etiologies. One of the main causes of retinitis is infectious agents. Viruses, bacteria, fungi and parasites can cause inflammation of the retina. For example, cytomegalovirus is often the cause of retinitis in immunocompromised individuals such as HIV/AIDS patients. Infections can enter the retina through the bloodstream or through nearby tissues of the eye.
Autoimmune diseases also play a significant role in the development of retinitis. In these cases, the immune system mistakenly attacks the retina's own cells, causing inflammation and tissue damage. This condition may be associated with systemic autoimmune diseases such as sarcoidosis or systemic lupus erythematosus.
Genetic factors can also cause retinitis. Some forms of retinitis, such as retinitis pigmentosa, are hereditary and passed from generation to generation. Mutations in certain genes can lead to the development of this disease, affecting the function of photoreceptors and other retinal cells.
Mechanism of development
The pathogenesis of retinitis involves a complex cascade of events that begins with the initial damage to retinal cells. When infectious agents penetrate the retina, they cause an acute inflammatory reaction. The immune system responds to the presence of pathogens by recruiting white blood cells and other protective cells to the site of infection. This process leads to the release of various inflammatory mediators, such as cytokines and chemokines, which exacerbates the inflammatory response.
In the case of autoimmune retinitis, the immune system attacks the healthy cells of the retina, perceiving them as foreign. This leads to chronic inflammation, which can cause permanent tissue damage. Over time, photoreceptors are destroyed, which negatively affects the ability to perceive light and transmit visual information to the brain.
Genetic forms of retinitis are usually associated with defects in genes that code for proteins necessary for normal retinal function. For example, mutations in the genes responsible for the structure and function of photoreceptors can lead to their degeneration. In such cases, the disease develops gradually, leading to a gradual loss of vision.
Classification of retinitis
Types of retinitis
Retinitis is classified according to several criteria, including etiology and clinical features. One of the most common types is retinitis pigmentosa, an inherited disease that leads to progressive degeneration of the retina. Infectious retinitis is caused by infectious agents such as viruses, bacteria, or fungi. Allergic retinitis develops due to allergic reactions to certain substances. There are also other forms of retinitis due to different causes, such as trauma or systemic diseases.
Clinical manifestations of each type
Retinitis pigmentosa usually begins with a gradual deterioration of night vision, which is a consequence of the loss of function of the rods - photoreceptors responsible for the perception of light in low light conditions. Over time, patients notice a narrowing of peripheral vision, which leads to so-called "tunnel vision". In the later stages of the disease, a significant decrease in central vision is possible, which makes it difficult to perform everyday tasks.
Infectious retinitis has various clinical manifestations, depending on the causative agent. For example, cytomegalovirus retinitis in immunocompromised patients may present with eye pain, decreased visual acuity, and floaters in the field of vision. Herpetic retinitis is often accompanied by pain and inflammation, and can lead to retinal detachment, which requires immediate medical intervention.
Allergic retinitis usually appears seasonally or after contact with allergens. Patients complain of itching, redness of the eyes and swelling of the eyelids. Decreased vision due to retinal edema is possible, although this condition is usually temporary and improves after elimination of the allergen and the use of anti-inflammatory drugs.
Other forms of retinitis may have specific symptoms depending on their cause. For example, traumatic retinitis is often accompanied by sudden vision loss, pain, and retinal hemorrhages. Retinitis associated with systemic diseases such as diabetes or vasculitis may present with progressive loss of vision, retinal hemorrhages, and macular edema.
Diagnosis of retinitis
Diagnostic methods
Diagnosis of retinitis is a complex process that requires the use of modern technologies and a thorough examination of the patient. One of the most important methods is ophthalmoscopy, which allows the doctor to examine the retina in detail. During the procedure, the doctor uses a special device - an ophthalmoscope, which allows you to see the internal structures of the eye. This helps to detect signs of inflammation, swelling, hemorrhages or other pathological changes in the retina.
Fluorescence angiography is another important diagnostic method. It includes the introduction of a fluorescent dye into the patient's vein and subsequent photography of the retina with a special camera. This makes it possible to detect impaired blood circulation in the retina and to identify areas of inflammation or damage.
Electroretinography (ERG) is used to assess retinal function. This method measures the electrical activity of photoreceptors in response to light stimuli. It is useful for determining the extent of retinal damage, especially in cases of retinitis pigmentosa, where the photoreceptors gradually lose their function.
Genetic testing may be helpful in cases of suspected hereditary forms of retinitis. DNA analysis allows detecting mutations in genes associated with the disease, which helps to confirm the diagnosis and determine the prognosis for the patient.
Differential diagnosis
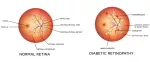
Differential diagnosis of retinitis is an important stage in the process of establishing an accurate diagnosis. It includes the exclusion of other retinal diseases that may have similar clinical manifestations. One such condition is diabetic retinopathy, which can cause swelling and hemorrhages in the retina similar to retinitis. A careful history and additional tests, such as blood sugar measurements, help distinguish between these conditions.
Another disease that needs to be ruled out is retinal detachment, which can be accompanied by a sudden loss of vision and the appearance of floating objects in the field of vision. Ophthalmoscopy and fluorescein angiography help detect detachment and distinguish it from inflammatory processes in retinitis.
Inflammatory conditions such as uveitis can also have similar symptoms, including soreness, redness of the eye, and decreased vision. An important aspect of differential diagnosis is the determination of the localization of the inflammatory process and its spread to other structures of the eye, which can be detected using ophthalmoscopy and ultrasound.
Treatment of retinitis
Drug therapy
Treatment of retinitis begins with drug therapy, which is aimed at reducing inflammation and preventing further damage to the retina. Depending on the cause of retinitis, different groups of drugs are used. Anti-inflammatory drugs, such as corticosteroids, are the main means of reducing the inflammatory process. They can be prescribed in the form of drops, tablets or injections. In infectious retinitis caused by bacteria or viruses, antibiotics or antiviral drugs are used, respectively. In cases of autoimmune retinitis, immunomodulatory drugs are prescribed to help control the activity of the immune system.
Surgical treatment
In cases where drug therapy does not bring the desired result or the disease progresses, surgical intervention may be necessary. One of the methods is vitrectomy, an operation in which the vitreous body of the eye is removed, which allows access to the retina and removal of inflammatory cells or restoration of its integrity. This procedure is also used to remove hemorrhages or scars that may form as a result of the inflammatory process. Laser coagulation is another surgical technique used to fix the retina in place and prevent it from further detachment. Laser coagulation can also be used to treat newly formed blood vessels that can cause retinal hemorrhages.
Innovative methods of treatment
Modern medicine is actively developing new methods of treating retinitis, which are aimed at restoring the functions of the retina and preventing vision loss. One of the promising directions is gene therapy. This approach consists of introducing healthy copies of genes into retinal cells to correct the genetic defects that lead to the development of retinitis. Gene therapy has already shown encouraging results in the treatment of some forms of retinitis pigmentosa.
Another innovative method is the use of stem cells. These cells have the ability to differentiate into different cell types, including photoreceptors. The introduction of stem cells into the retina can help restore damaged tissue and improve vision. Although these methods are still in the research stage, they open new perspectives for the treatment of retinitis in the future.
Prevention and prognosis
Preventive measures
Prevention of retinitis includes several important aspects that help reduce the risk of developing the disease and preserve the health of the retina. Regular eye exams are a key element of prevention, especially for people at increased risk, such as patients with chronic conditions such as diabetes or hypertension. Early detection of inflammatory processes in the retina allows timely treatment and prevention of complications.
A healthy lifestyle also plays an important role in preventing retinitis. A balanced diet rich in antioxidants, vitamins A, C and E promotes the health of the retina. It is also important to avoid smoking, as the nicotine and toxins in tobacco can damage the blood vessels in the retina.
For patients with a genetic predisposition to retinitis, genetic counseling is an important preventive measure. It allows you to assess the risk of disease development in future generations and take the necessary measures to reduce this risk. In some cases, regular genetic testing may be recommended for early detection of mutations that lead to retinitis.
Prognosis for patients
The prognosis for patients with retinitis largely depends on the type and stage of the disease, as well as on the timeliness and effectiveness of treatment. For example, retinitis pigmentosa usually has a progressive nature, but early diagnosis and appropriate therapy can significantly slow down the development of the disease and preserve vision for a long time. Infectious retinitis, with timely detection and treatment with antibiotics or antiviral drugs, can have a favorable prognosis, with the possibility of full recovery or significant improvement of the condition.
Autoimmune retinitis requires constant monitoring and control with immunomodulatory therapy. With effective treatment, it is possible to stabilize the condition and prevent further damage to the retina. However, in cases where the disease has already led to significant structural changes in the retina, the prognosis may be less favorable, and efforts will be made to preserve residual vision.
Innovative treatments, such as gene therapy and the use of stem cells, open new perspectives for improving the prognosis of patients with genetic forms of retinitis. Although these methods are still in the research stage, they show encouraging results and may be the key to effective treatment in the future.